Visualization of adrenal tumors using near-infrared autofluorescence
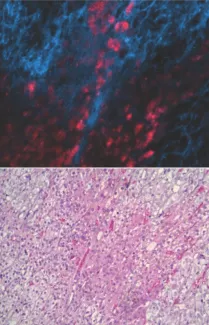
Adrenal tumor cells can be detected by illumination with near-infrared light. Invasive adrenal tumor cells in a background of normal tissue exhibit red fluorescence (top image) when illuminated with near-infrared light, while normal cells are shown in blue. Visualization of the signal does not require any processing or staining of the tissue specimen. The bottom image is a conventional stained and processed tissue section of the same tumor.
Detection of near-infrared (NIR) autofluorescence in human tissues in situ is a recently developed technique. The only current FDA-approved usage is for intraoperative visualization of the parathyroid glands in order to avoid inadvertent injury during anterior neck surgery. The parathyroid glands are currently the only human tissue known to exhibit intrinsic NIR autofluorescence. We studied this phenomenon and observed that NIR autofluorescence originated in a subset of large, lipid-positive granules distinct from adipose tissue or the smaller, more numerous intracellular secretory granules associated with parathyroid hormone secretion. Because these larger granules resembled the lipid bodies found in the adrenal cortex, we hypothesized that adrenal tissue might also be NIR autofluorescent. In preliminary studies, we have found that the adrenal cortex emits strong, intrinsic NIR autofluorescence. In a pilot panel of adrenal neoplasms, benign adrenocortical adenomas were non-fluorescent while adrenocortical carcinomas contained clusters of brightly fluorescent cells, suggesting that NIR evaluation could be a useful adjunct to existing cytomorphological criteria in making this critical and challenging diagnostic distinction. In this project, we are assessing whether visualization of adrenal tumor autofluorescence may have clinical utility. We are examining adrenal tissue from a range of pathological states (functional and non-functional adrenocortical tumors; pheochromocytomas; adrenocortical carcinomas, lymph node metastases) to determine the range and variability of NIR signal intensity and evaluate its potential utility as a diagnostic classification tool. These data will identify specific clinical contexts where NIR illumination would most likely be informative. If validated, intraoperative visualization of adrenal gland NIR autofluorescence in real time could significantly improve cytopathological diagnosis, establish a rapid and direct intraoperative observation method for assessment of tumor margins and possible lymph node involvement, and provide a powerful tool for detecting residual disease and confirming completion of tumor resection.
This work is supported by a grant from the Mount Zion Health Fund (MZHF #20211336/#20201225)
